Whatever your age, it’s good to get into the habit of checking. The risk of breast cancer increases with age, so if you are over 50, you’ll get an invitation for free breast screening every three years up to the age of 70. And remember if you’re over 70 you are still entitled to free breast screening – just ask your doctor.
Breast cancer is the most common cancer among women, after skin cancer. It is also the second leading cause of cancer death in women after lung cancer. Encouragingly, the death rate from breast cancer has declined a bit in recent years, perhaps due to greater awareness and screening for this type of cancer, as well as better treatments.
Breast cancer is the most common cancer among women, after skin cancer. It is also the second leading cause of cancer death in women after lung cancer. Encouragingly, the death rate from breast cancer has declined a bit in recent years, perhaps due to greater awareness and screening for this type of cancer, as well as better treatments.
Breast cancer is a disease that occurs when cells in breast tissue change (or mutate) and keep reproducing. These abnormal cells usually cluster together to form a tumor. A tumor is cancerous (or malignant) when these abnormal cells invade other parts of the breast or when they spread (or metastasize) to other areas of the body through the bloodstream or lymphatic system, a network of vessels and nodes in the body that plays a role in fighting infection.
Breast cancer usually starts in the milk-producing glands of the breast (called lobules) or the tube-shaped ducts that carry milk from the lobules to the nipple. Less often, cancer begins in the fatty and fibrous connective tissue of the breast.
New cases of breast cancer are about 100 times more common in women than in men, but yes, men can get breast cancer too. Male breast cancer is rare, but anyone with breast tissue can develop breast cancer.
Breast cancer is caused by a genetic mutation in the DNA of breast cancer cells. How or why this damage occurs isn’t entirely understood. Some mutations may develop randomly over time, while others are inherited or may be the result of environmental exposures or lifestyle factors.
Some breast cancer risks may be preventable. Of course, you cannot control every variable that may influence your risk. Here are the key breast cancer risk factors to know.
Age and gender.
If you are a woman and you’re getting older, you may be at risk of developing breast cancer. The risk begins to climb after age 40 and is highest for women in their 70s.
Family history.
Having a close blood relative with breast cancer increases your risk of developing the disease. A woman’s breast cancer risk is almost double if she has a mom, sister, or daughter with breast cancer and about triple if she has two or more first-degree relatives with breast cancer.
A breast cancer gene mutation.
Up to 10% of all breast cancers are thought to be inherited, and many of these cases are due to defects in one or more genes, especially the BRCA1 or BRCA2 genes. (Scientists are studying several other gene mutations as well.) In the U.S., BRCA1 and BRCA2 mutations are more common in Jewish women of Eastern European descent. Having these defective genes doesn’t mean you will get breast cancer, but the risk is greater: A woman’s lifetime risk of breast cancer with a BRCA1 gene mutation, for example, may be more like 55% to 65% compared to the average 12%.
Breast changes and conditions.
Women with dense breasts or with a personal history of breast lumps, a previous breast cancer, or certain non-cancerous breast conditions are at greater risk of developing breast cancer than women who do not have these conditions.
Race/ethnicity.
White women are slightly more likely to develop breast cancer than Asian, Hispanic, and African American women. But African American women are more likely to develop more aggressive breast cancer at a younger age and both African American and Hispanic women are more likely to die from breast cancer than white women.
Hormones.
Women with early menstrual periods (starting before age 12) and late menopause (after age 55) are at greater risk of getting breast cancer. Scientists think their longer exposure to the female hormone estrogen may be a factor, because estrogen stimulates growth of the cells of the breast. Likewise, use of hormone therapy after menopause appears to boost the risk of breast cancer. Oral birth control pills have been linked to a small increase in breast cancer risk compared with women who never used hormonal contraception. But that risk is temporary: More than 10 years after stopping the pill, a woman’s breast cancer risk returns to average.
Weight.
Women who are overweight or obese after menopause are more likely to get breast cancer. The exact reason why isn’t clear, but it may be due to higher levels of estrogen produced by fat cells after menopause. Being overweight also boosts blood levels of insulin, which may affect breast cancer risk.
Alcohol consumption.
Studies suggest women who drink two or more alcoholic beverages a day are 1 1/2 times more likely than non-drinkers to develop breast cancer. The risk rises with greater alcohol intake, and alcohol is known to increase the risk of other cancers too. For that reason, the American Cancer Society (ACS) recommends that women stick to one drink a day–or less.
Radiation exposure.
A woman’s risk of developing breast cancer may be higher than normal if she had chest radiation for another disease as a child or young adult.
Pregnancy history.
Having no children or having a first child after age 30 may increase your risk of breast cancer.
Researchers have identified four main types:
TOUCH
Can you feel a lump? Either in the breast, upper chest or armpits.
Is there a lumpy area? Or unusual thickening of the breast tissue that doesn’t go away?
Is there any unusual pain? Either in part of the breast or the armpit
LOOK
Any change in size or shape? e.g. one breast might become larger or lower than the other
Any change in skin texture? Such as puckering or dimpling of the skin of the breast
Any change in colour? e.g. the breast may look red or inflamed
What about the appearance or direction of the nipple? e.g. one might become inverted (turned in) when it normally points out
Any unusual discharge? One or both nipples might have a discharge.
Any rash or crusting? Of the nipple or surrounding area
CHECK
Is anything unusual? If so, get it checked out by your doctor as soon as possible
You may normally feel breast tissue changes or pain before or during your periods. This is why it’s important to check your breasts regularly so you get to know how they look and feel at different times of the month, and can notice any changes that are unusual for you.
Yes, it does, though the specifics are hard to pinpoint. There are four studies worth noting. A large-scale analysis of nearly 150,000 women published in The Lancet in 2002 found that for every 12 months of breastfeeding (either with one child or spread over multiple children), the risk of breast cancer decreased by 4.3 percent, when compared to women who didn't breastfeed at all.
Then a 2009 study of more than 60,000 women published in the Archives of Internal Medicine found that women with a family history of breast cancer reduced their risk of getting the disease before menopause by nearly 60 percent if they breastfed.
A study published this year by the Journal of the National Cancer Institute found that women of African ancestry have an especially high risk of developing the aggressive and hard-to-treat forms of breast cancer called estrogen receptor-negative and triple-negative—and the risk actually goes up when a woman gives birth—but breastfeeding negates this risk.
If you find a lump or other change in your breast — even if a recent mammogram was normal — make an appointment with your doctor for prompt evaluation.
Making changes in your daily life may help reduce your risk of breast cancer. Try to:
Ask your doctor about breast cancer screening.
Become familiar with your breasts through breast self-exam for breast awareness.
Avoide Alcohol
Exercise most days of the week
Limit postmenopausal hormone therapy.
Maintain a healthy weight.
Ductal carcinoma in situ (DCIS)
This highly treatable pre-cancer (sometimes called “stage 0” breast cancer) starts in a milk duct. It’s the most common type of non-invasive breast cancer, meaning the cells are abnormal but haven’t spread to the surrounding tissue. Over time, DCIS may progress to invasive breast cancer.
Invasive ductal carcinoma (IDC)
This is the most common breast cancer, accounting for 80% of all invasive breast cancer diagnoses. Also called “infiltrating ductal carcinoma,” IDC starts in a milk duct, breaks through the duct wall, and invades the surrounding breast tissue. It can spread to other parts of the body as well. There are also several subtypes of IDC, which are categorized based on features of the tumors that form.
Lobular carcinoma in situ (LCIS)
LCIS, also called lobular neoplasia, starts in the milk-producing lobules. Technically, it’s not breast cancer (even though it has carcinoma in its name), but rather a collection of abnormal cells. People with LCIS are more likely to develop breast cancer in the future.
Inflammatory breast cancer (IBC)
This rare, aggressive type of breast cancer causes redness and swelling of the breast. The affected breast can feel warm, heavy, and tender. The skin may become hard or ridged like an orange rind. See a doctor right away if you have these symptoms. Inflammatory breast cancer tends to strike five years earlier, on average, than other types of breast cancer, and it might not show up on a mammogram. African American women are at greater risk for IBC than white women.
Paget disease of the breast (or the nipple)
This rare cancer affects the skin of the nipple and the darker circle of skin, called the areola, surrounding it. People with Paget disease may notice the nipple and areola becoming scaly, red, or itchy. They may also notice yellow or bloody discharge coming from the nipple. Most people who have this condition also have one or more tumors (either DCIS or invasive cancer) in the same breast.
Metaplastic breast cancer
This rare, invasive breast cancer begins in a milk duct and forms large tumors. It may contain a mix of cells that look different than typical breast cancers and can be more difficult to diagnose.
Angiosarcoma of the breast
This quickly growing cancer is rare. It is usually a complication of a prior radiation treatment of the breast.
Its treatment depends on the stage of cancer. It may consist of chemotherapy, radiation, hormone therapy and surgery.
Surgery
Mammaplasty
Plastic surgery to increase or reduce the size of the breasts or to reconstruct a breast.
Tissue expansion
Inserting a balloon under the skin and then gradually expanding it to stretch and grow the skin and surrounding tissue.
Lymph node dissection
Surgical removal of a lymph node.
Lumpectomy
Surgical removal of a lump (tumour) in the breast.
Mastectomy
Surgical removal of some or all of the breast.
Medical procedure
Teletherapy
Radiation therapy that uses x-rays or other high-energy beams to destroy cancer cells and shrink tumours.
Radiation therapy
Treatment that uses x-rays and other high-energy rays to kill abnormal cells.
Even if you perform self-checks religiously, lumps cannot always be felt by the bare hand.
Mammograms can be fit easily into a busy schedule, taking as little as 20 minutes.
Breast cancer is the 2nd leading cause of death among American women; mammograms can help detect breast cancer at an early and easily treatable stage.
Being vigilant about breast cancer prevention sets a good, encouraging example for the other women in your life.
Of course. It’s incredibly important that women with breast augmentation continue to have mammograms. It is important to inform your doctor performing your mammogram that you have received implants so that they can adjust accordingly – even though implants may hide some breast tissue, your doctor should be experienced in performing mammograms on breast augmentation patients. Special techniques, like implant displacement views, are now being used to help detect abnormal tissue around the implant. Impant Displasment View is a procedure used to do a mammogram (x-ray of the breasts) in women with breast implants. The implant is pushed back against the chest wall and the breast tissue is pulled forward and around it so the tissue can be seen in the mammogram. Also called Eklund displacement views and Eklund views.
It’s all about not wearing anything that can affect the results of the test. These items should be avoided when going in for your scan:
Deodorantd
Lotion
Powder
Perfume
Jewelry
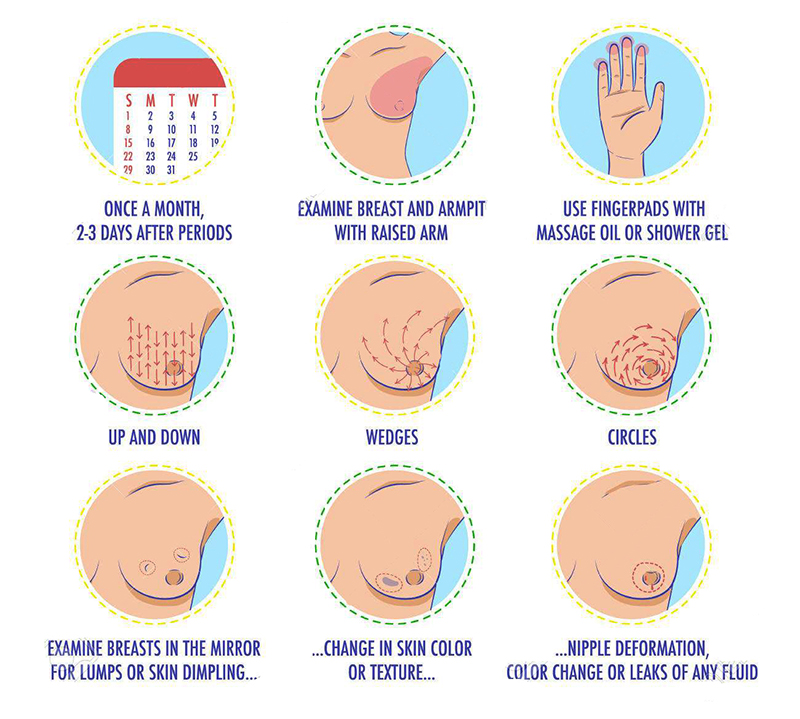
Breast Self Examination